GreyMatters
Educational articles, BetterBrain resources, latest in brain health, and news about us. Written for you, with expertise (and love).
Cholesterol and Your Brain: What You Actually Need to Know
Cholesterol gets a bad rap. For decades, we've heard that it clogs arteries and causes heart attacks. But here's what doesn't make headlines: your brain contains 25% of your body's total cholesterol despite making up only 2% of your body weight. As lipid expert Dr. Tom Dayspring puts it, "Cholesterol is almost certainly the most important molecule in the brain."
So how can cholesterol be both necessary for brain function and a major cardiovascular risk factor? The answer lies in understanding where cholesterol is, how it gets there, and what form it takes.
In this post, we're taking a deeper dive into cholesterol than usual. We'll break down what your cholesterol numbers actually mean, why the standard tests miss critical information, and how the cholesterol story connects cardiovascular health to brain health.
The Basics: What Is Cholesterol?
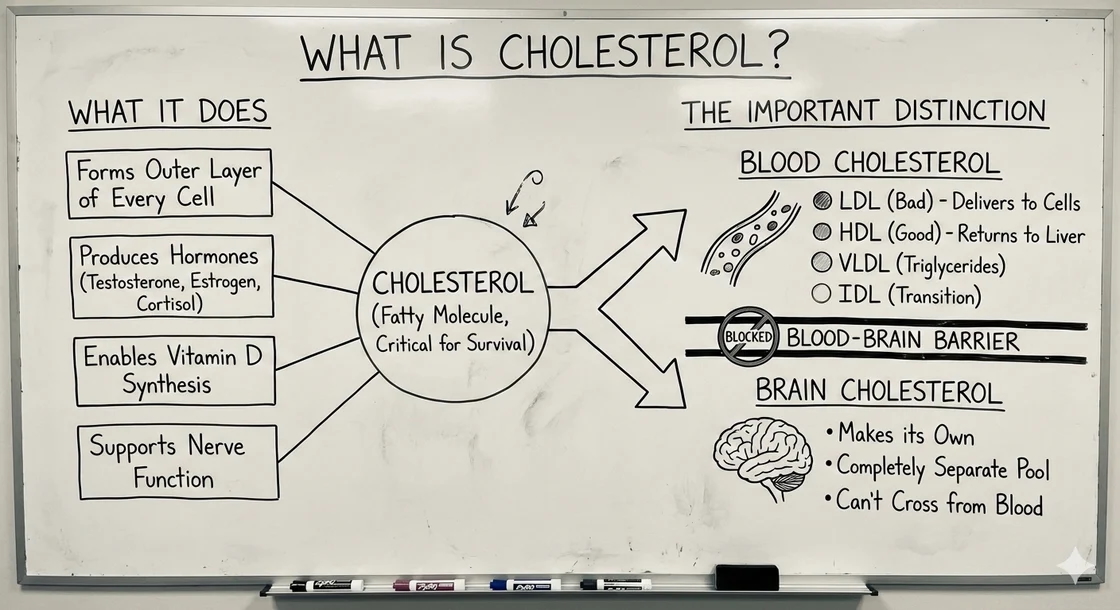
Cholesterol is a fatty molecule that serves critical functions throughout your body. It forms the outer layer of every cell, helps produce hormones (including testosterone, estrogen, and cortisol), enables vitamin D synthesis, and supports nerve function. Without cholesterol, you simply couldn't survive.
But there's an important distinction to make: "cholesterol" isn't one thing.
When we talk about cholesterol in the blood versus cholesterol in the brain, we're really talking about two separate systems that operate differently.
Blood cholesterol: Cholesterol travels through your bloodstream inside particles called lipoproteins. These particles come in different types:
- LDL (low-density lipoprotein): Often called "bad" cholesterol, LDL particles deliver cholesterol to cells throughout your body
- HDL (high-density lipoprotein): Called "good" cholesterol, HDL particles help transport excess cholesterol back to the liver
- VLDL (very low-density lipoprotein): Primarily transports triglycerides but also carries some cholesterol
- IDL (intermediate-density lipoprotein): A transition form between VLDL and LDL
Brain cholesterol: Your brain makes its own cholesterol and keeps it completely separate from blood cholesterol. The blood-brain barrier prevents cholesterol in your bloodstream from entering your brain. This means the cholesterol circulating in your blood and the cholesterol in your brain are part of two entirely different pools.
The Heart Risk: Why apoB Matters More Than LDL?
What is apoB?
ApoB (apolipoprotein B) is a protein found on the surface of all atherogenic (plaque-forming) particles, including LDL, VLDL, IDL, and Lp(a). Each particle contains exactly one apoB molecule, making apoB a direct count of total potentially harmful particles.
Why apoB beats LDL cholesterol?
Traditional LDL-C (LDL cholesterol) tells you how much cholesterol LDL carries, but not how many particles you have. Two people can have identical LDL-C but vastly different particle numbers and risk levels.
- Many small LDL particles (each carrying less cholesterol) = "normal" LDL-C but high particle count and high risk
- Fewer large LDL particles (each carrying more cholesterol) = higher LDL-C but fewer particles and potentially lower risk
ApoB counts every atherogenic particle regardless of size. This makes it the best single marker for cardiovascular risk.
What is the triglyceride connection?
Elevated triglycerides (often from insulin resistance) fundamentally alter lipid metabolism:
- VLDL becomes triglyceride-enriched
- Particles get remodeled into small, dense LDL
- ApoB particle count increases
- You can have "normal" LDL-C but dangerously high apoB
This is why metabolic health is critical for cardiovascular risk.
The Brain Side: Why Cholesterol Is Essential
While high apoB threatens your heart, brain cholesterol is absolutely essential.
Critical brain functions
- Myelin formation: Insulates nerve fibers for rapid signal transmission
- Synapse formation: Creates and maintains neuron connections
- Cell membranes: Every neuron needs cholesterol-rich membranes
- Neurotransmitter release: Regulates how neurons communicate
How the brain gets cholesterol
Astrocytes (brain cells) produce cholesterol and package it into brain-specific lipoproteins containing apoE (apolipoprotein E) for delivery to neurons.
The APOE genetic factor
- APOE ε2: Protective against Alzheimer's, better cholesterol handling
- APOE ε3: Most common, considered neutral
- APOE ε4: Increases Alzheimer's risk, disrupts brain cholesterol metabolism
Research from MIT shows APOE4 is associated with brain cells accumulating cholesterol abnormally rather than using it to make healthy myelin. This isn't about too much or too little cholesterol, but how effectively the brain uses it.
Cholesterol and Alzheimer's
Brain regions vulnerable to Alzheimer's show signatures of being "super cholesterol-hungry," as researchers describe it, constantly trying to produce and absorb cholesterol. When this system fails (especially with APOE4), neurodegeneration may follow.
The Paradox Resolved
In the bloodstream: High apoB drives atherosclerosis. Particles penetrate artery walls, oxidize, trigger inflammation, form plaques. Goal: Keep apoB low (<60-80 mg/dL) to prevent cardiovascular disease.
In the brain: The brain makes its own cholesterol independently. Blood cholesterol can't cross the blood-brain barrier. Goal: Support healthy brain cholesterol metabolism through metabolic health.
This separation means lowering blood cholesterol doesn't starve your brain. Your brain continues making what it needs regardless of apoB levels.
The Bottom Line
Cholesterol isn't inherently good or bad; context is everything. In your bloodstream, high apoB poses serious cardiovascular and cerebrovascular risks. In your brain, cholesterol is essential for structure and function.
The good news: these systems are separate. Lowering apoB to protect your heart doesn't harm your brain. In fact, protecting your cardiovascular system through better lipid management, metabolic health, and inflammation control also protects your brain.
Understanding which biomarkers matter empowers informed decisions. It's not about fearing cholesterol; it's about managing it intelligently.
Want to Understand Your Complete Lipid Profile and Genetic Risk?
BetterBrain includes apoB, advanced lipid testing, metabolic biomarkers, and APOE genetic testing for a complete cardiovascular and brain health picture.

Unlocking the Power of Omega-3 Fatty Acids
As the quest for effective Alzheimer’s prevention continues, recent studies1,2 underscore the profound impact of dietary choices on our brain health. One nutrient class consistently at the forefront of neuroprotective research is Omega-3 fatty acids, particularly Docosahexaenoic Acid (DHA) and Eicosapentaenoic acid (EPA). In this post, we explore how integrating DHA and EPA into your diet can play a crucial role in reducing the risk of Alzheimer's disease.
Fatty acids explained1
DHA and EPA are a major omega-3 fatty acid predominantly found in fish oils. They are called essential fatty acids, meaning that the human body cannot produce them on its own, so they must come from dietary sources. Make sure not to confuse omega-3s (like DHA and EPA) with omega-6s. These are a different class of fatty acids typically found in vegetable oils and nuts. They are much more common in most diets, and can promote inflammation when consumed in excess.
DHA and EPA are particularly important because the molecules are building blocks for neurons. This means that maintaining healthy levels of DHA and EPA supports neuronal membrane integrity, promotes healthy synaptic activity, and mitigates inflammation within the brain. Long-term, these fatty acids have been shown to help preserve cognitive abilities and delay the onset of dementia1.
Clinical insights on Alzheimer’s prevention
A growing body of research points to a direct correlation between DHA and EPA intake and a reduction in the risk for Alzheimer's. Animal studies provide compelling evidence, showing that diets rich in DHA can significantly reduce the formation of amyloid plaques, which are closely linked to Alzheimer’s pathology1.
Furthermore, in human epidemiological research (research that investigates the distributions and determinants of health-related events in populations), increased consumption of DHA through dietary sources like fish has been associated with lower incidence rates of Alzheimer’s, suggesting its significant protective effect. One study3 found that people with the highest levels of DHA had a 49% lower risk of developing Alzheimer's disease compared to those with the lowest levels. This means that those in the top 20% were about half as likely to get Alzheimer's as those in the bottom 20%. Additionally, increasing DHA levels from the lowest group to the highest group was predicted to give an extra 4.7 years of life free from Alzheimer's disease.
Other studies have concluded similar results, showing a 47%5 reduction in risk, though there is debate about when this effect may occur. The consensus is that DHA supplementation is most effective when started early, before symptoms get classified as dementia6.
Increasing your omega-3 intake
There are two main ways to make sure you’re getting enough DHA and EPA - either making conscious dietary choices4 or taking supplements. From the diet side, fatty fish are an excellent source of omega-3s. Typical guidance recommends eating fish like salmon, mackerel, herring, or halibut at least 3 times per week. It’s worth noting that chia seeds and flax seeds are also excellent sources of omega-3s. Predatory fish like tuna are also good sources of EPA and DHA, but be careful not to consume them too often since they also contain high levels of mercury.
Fish oil supplements can be another great way to increase your intake of omega-3s - if you carry the APOE4 gene, supplementation is particularly important since you may have more trouble absorbing dietary omega-3s. However, it’s important to recognize that not all supplements were created equal. Specifically, not all brands will have the same purity of fatty acids, and not all will contain sufficient levels of DHA and EPA. Here are some things to look out for to make sure you are getting high quality fish oil:
- High amounts of DHA and EPA per serving (at least 500mg combined per serving)
- Minimal additives in the ingredients other than the oil and capsule contents
- Packaged in dark containers to protect the oil from light
A Step Towards Cognitive Longevity
Embracing a diet that includes adequate amounts of DHA and EPA can significantly contribute to brain health and potentially decrease the risk of Alzheimer’s. Start by evaluating your current dietary habits and consider how you might improve your omega-3 intake, ensuring your brain remains vibrant and healthy well into later life.
Where to get started
- Measure your blood omega-3 index to learn your current EPA and DHA levels. This is one of the 50+ biomarkers tested during your BetterBrain Essentials blood draw.
- Eat at least 3 servings of fatty fish (e.g., salmon, mackerel) per week, but make sure not to overdo your intake of predatory fish like tuna.
- Consider using fish oil supplements to increase your EPA and DHA intake. We recommend Carlson’s fish oil, which is available at a discount with a BetterBrain membership.
The Role of Homocysteine in Dementia Risk
Homocysteine is a naturally occurring amino acid in our body and can spike acutely, such as after staying up all night. In healthy people, homocysteine naturally clears over time. However, at chronic high concentrations, it is associated with various health issues, including heart disease and, notably, cognitive decline. In fact, having blood homocysteine levels over 14 μmol/L is associated with a nearly doubled risk of dementia1. Luckily, there are simple ways to lower your homocysteine levels - most notably B vitamin supplementation.
Brain Atrophy, Aging and Cognitive Decline
As we age, our brains naturally undergo some amount of atrophy, or decrease in size, which involves a loss of neurons and their connections. This process is accelerated in Alzheimer’s dementia2. With a lower brain volume and fewer neural connections, it’s easy to see how atrophy can lead to lasting cognitive impairment. One factor that has a strong influence on the rate of brain atrophy is blood concentration of homocysteine. Several studies3,4 link elevated homocysteine levels are linked with a heightened risk of dementia.
The role of B vitamins
You won’t often hear us say this, but you have an ace up your sleeve in fighting homocysteine: B vitamins. One study2 investigated the effects of using B6, B9, and B12 vitamins over the course of two years, using the same level of rigor that is commonly used for drug clinical trials.
On average, people who used B vitamins lowered their overall homocysteine levels by 32% and experienced a 30% slower rate of brain atrophy. In fact, those who started with very high levels of blood homocysteine (> 14 μmol/L) managed to slow their atrophy rate by 53%. In other words, this study suggests that the simple act of taking a daily B vitamin supplement can cut your dementia risk in half.
The type of B vitamin matters
There are two factors to consider when selecting a B vitamin supplement. The first is what vitamins you are getting. The study mentioned above specifically tested the use of vitamins B6, B9 (also known as folate), and B12. It’s important to get a mix of both. The second is whether or not you select the methylated form of the vitamins. Methylation is a biological process that makes the vitamins more available for your body to use. In other words, the same dose of methyl-B vitamins will be more strongly absorbed than normal B vitamins. This is especially important for people with mutations in the MTHFR gene, since they otherwise have trouble absorbing B vitamins. We generally recommend taking methylated B vitamins since they are perfectly safe, but if you are sensitive to overmethylation, you may want to consider regular B vitamins to avoid side effects like headaches, anxiety, or irritability.
Broader Implications for Dementia Prevention
Homocysteine is a critically important risk factor for dementia. Not only does it accelerate brain atrophy, it also aggravates other conditions through inflammation and oxidative stress. Thankfully, B vitamins are an extremely effective tool to lower homocysteine levels. While there are many other ways of managing your homocysteine levels, most notably through diet, exercise, and stress management, B vitamins are a low-effort high-impact way to keep your brain atrophy at bay.
Get started on managing your homocysteine
- Measure your blood homocysteine levels to learn where you stand. Homocysteine is one of the 50+ biomarkers tested during your BetterBrain Essentials blood draw.
- Consider using B vitamin supplements to lower your homocysteine, ideally below 9 μmol/L. We recommend Pure Encapsulations MethylAssist, but make sure you use an unmethylated alternative if you are sensitive to overmethylation.
- Learn more about homocysteine on the Peter Attia Drive episode on dementia. This episode covers many topics, so if you’re just interested in homocystine, skip ahead to 1:09:00.

Rapamycin: Revolutionizing Alzheimer's Prevention?
In the 1960s, researchers on Easter Island were investigating local indigenous peoples’ claims that the soil has healing properties. After testing various soil samples, the researchers isolated a small molecule they believed was responsible for the effects. They named it rapamycin5, after the traditional name for the island, Rapa Nui. Since its discovery, rapamycin has been used in various settings, from an antifungal agent to more recently a beacon of hope in anti-aging medicine. Additionally, it is showing promise in extending lifespan and preventing neurodegenerative diseases such as Alzheimer’s.
From anti-rejection med to longevity enhancer
The transition from an antifungal to a potential longevity drug has been intriguing. Rapamycin, approved in 1999 for its immunosuppressant qualities, is still commonly used in kidney transplants to prevent organ rejection. However, a 2014 study1 on older adults revealed a paradox: at much smaller doses, rapamycin boosted the immune response to flu vaccinations, despite their age-related weakened immune function. This unexpected enhancement suggests that rapamycin might have broader applications for disease prevention in older adults, potentially making it a valuable tool in combating age-related declines in the human immune system.
How rapa works
To understand how rapamycin works, it’s important to understand the molecule that it targets: a cellular receptor named mTOR. mTOR is present in nearly all cells in the human body and is responsible for mediating pathways that regulate cell growth, metabolism, and survival. Inhibiting mTOR completely is catastrophic - it prevents cells from making energy, eventually leading to their death. However, partial inhibition means that mTOR has a harder time forming a cluster with other proteins, which makes the cell act as if it's not getting enough food. This starts a process where the cell breaks down unneeded or damaged parts, like proteins that aren't folded correctly, which can otherwise impair the cell’s ability to function. This leads to improved cellular survival and resilience and is particularly relevant to brain health since one of the main features of Alzheimer’s is the accumulation of misfolded amyloid beta protein plaques in neurons.
The partial inhibition of mTOR therefore shows potential for slowing down the progression of Alzheimer’s disease and improving the survival rate of neurons. Animal studies2,3 suggest that rapamycin may help mitigate or improve many of the pathologies associated with Alzheimer's disease and potentially restore cognitive function.
Growing evidence yet limited human trials
While animal studies have robustly demonstrated lifespan and healthspan extensions—with remarkable outcomes like a 20-30% increase in the lifespan of mice4—human data remains scarce. The gap in human trials can be largely attributed to the fact that rapamycin use for longevity is considered “off-label”. This means that the Federal Drug Administration (FDA) has not yet approved rapamycin for this use, which diminishes incentives for comprehensive research funding. However, the evidence from animal studies across a variety of species strongly suggests a significant potential for rapamycin in anti-aging treatments.
Rapamycin’s mainstream use
As mentioned earlier, the FDA has only approved rapamycin for use as an immunosuppressant. It’s important to recognize that rapamycin use for longevity is still considered experimental and will not be reimbursed by insurance. Because the FDA hasn’t established guidelines around its use, there is no single accepted protocol for rapamycin dosage. Given the drug’s complex effects, the risk of experiencing side effects is real. Nonetheless,many individuals already use rapamycin “off-label” under the supervision of a physician for its longevity benefits. This is a perfectly legitimate use of the molecule, even though there is a lot we have yet to learn.
A promising option for the future
Rapamycin offers a compelling glimpse into the future of longevity and neuroprotection. Although its journey from a soil sample to a potential anti-aging miracle has been gradual, the promise it holds could change the landscape of preventive health. As research continues, both the medical community and potential users must weigh the benefits against the uncertainties of translating animal model successes to human health outcomes.
Learn more
Listen to the Peter Attia Drive episode on rapamycin to learn more about the molecule, its history, how it works, and the most recent evidence on its effects.

Dietary Defenders: Prebiotic Fibers in Alzheimer's Prevention
As Alzheimer's disease continues to impact millions globally, the scientific community is increasingly focusing on the gut-brain axis. This complex communication network, which links the gastrointestinal tract and the brain, could play a major role in preventing cognitive decline. Recent discoveries1 have shown that gut microbiota might affect everything from brain development to behavior to disease states, and researchers are starting to explore how the gut-brain axis can influence dementia risk.
Exploratory study: A closer look at fiber's impact on aging brains
The School of Life Course & Population Sciences at King’s College London spearheaded a pivotal double-blind study2 (the same type of study as used for clinical trials) with participants over 60 years old. Their research aimed to uncover the cognitive effects of consuming prebiotic fibers compared to a placebo.
Fiber fuels cognitive fortitude
Like any organism, the components making up the gut microbiome need food to survive. One source of nutrients for them is prebiotic fibers, such as inulin and fructooligosaccharides (FOS), both of which were the focus of the King’s College study. The researchers found that participants who took prebiotic supplements had more of one species of healthy bacteria called Bifidobacterium in their gut. This species has previously been linked to better cognitive performance, and indeed the participants who took supplements showed improved cognitive function scores through the same memory tests that are used as an early indicator of Alzheimer’s disease.
Why is this happening?
The composition of the gut microbiome has drastically changed over human history. Advances in agriculture, industrialization and globalization may have caused a decrease in gut microbial diversity, which has been associated with worse health outcomes. In particular, a review of multiple studies1 suggests that changes in the microbiome can lead to behavioral changes. In another study3 comparing 25 patients diagnosed with Alheimer’s disease to 25 healthy individuals, those with Alzheimer’s were found to have reduced gut microbial diversity.
Keeping an eye on your intake
Let’s get specific. Women should aim to consume 21-25g of fiber per day. Men should aim for 30-38g4. Here is a list of some common fiber-dense foods to consider adding into your diet.

A promising path to cognitive health
Emerging evidence connecting dietary habits, gut microbiota, and brain function highlights a novel approach to combat Alzheimer’s disease. The gut-brain axis is still a new area of research - there is much we don’t know, and many researchers around the world are investigating the different ways in which the microbiome influences our brain health. Such studies not only pave the way for innovative therapeutic avenues but also emphasize the profound impact our diet can have on mental and overall health.
Putting the science in action
- Eat enough fiber each day to make sure you are nourishing your gut microbiome. Women should strive for 21-25g daily, while men should aim for 30-38g.
- Learn more about the importance of your gut health on your brain and body through the Peter Attia Drive podcast.some text
- Episode #215 goes in-depth on the GI system - skip to 34:30 for ways in which the gut and brain communicate, and to 1:55:00 for ways to promote your gut microbiome using your nutrition.
- Episode #283 discusses the microbiome specifically - learn more about the importance of fiber at 38:30 and about the gut-brain axis at 50:15.

Metabolic Syndrome as a Gateway to Dementia
It’s a well-known fact that Alzheimer’s disease is closely linked to metabolic health, to the point that some experts have begun to refer to it as Type III Diabetes. But what many people don’t know is that poor metabolic health is a strong risk factor for dementia long before it progresses to diabetes, even for people without a family history.
Decoding metabolic syndrome
Before you get diagnosed with diabetes, your body goes through a number of changes. Cells in your body become desensitized to insulin, which usually tells them to absorb sugar from your bloodstream. This results in chronically elevated blood sugar and in turn starts causing problems for your heart, liver, brain, and other organs. This pre-diabetic phase is called metabolic syndrome, and it affects ~25% of adults worldwide, including 40% adults aged 60+ in the U.S. Most of them do not know that metabolic syndrome is a health risk.
Metabolic syndrome is diagnosed when an individual has three or more of the following:
- High triglycerides (≥150 mg/dL)
- Elevated blood pressure (≥130 mmHg systolic or ≥85 mmHg diastolic) OR use of antihypertensive medication
- High fasting glucose (≥100 mg/dL OR use of glucose lowering medications)
- Low HDL cholesterol (<40 mg/dL in men; <50 mg/dL in women OR use of lipid-modifying medication)
- Abdominal obesity (waist circumference ≥102 cm for men and ≥88 cm for women)
It’s worth noting that hemoglobin A1c (HbA1c), a common marker for diabetes, does not feature on this list. Although a doctor won’t use A1c to diagnose metabolic syndrome, it’s still an important marker to keep track of your metabolic health.
Connecting metabolic syndrome to brain health
A large retrospective study1 analyzed data from 175,000 participants over a period of 15 years. Participants were aged 60+ and represented a variety of sociodemographic, lifestyle, and genetic backgrounds. With regards to the metabolic syndrome diagnosis criteria listed above, the study found that:
- Having three conditions increases dementia risk 12%
- Having four to five conditions is associated with an even stronger risk
- The link between metabolic syndrome and dementia is particularly strong in individuals who do not carry the APOE ε4 allele (typically, these are individuals with a lower risk of dementia)
Taking action
The first step is to know where you stand. It’s important to establish a baseline by measuring metabolic markers in your blood and potentially using a continuous glucose monitor (CGM) to see how your blood sugar reacts to your daily habits. This will help you make an informed decision on how to approach your metabolic health.
Metabolic health is strongly tied to your lifestyle - particularly your diet, physical activity, and sleep. There’s also several different drugs, like statins or ACE inhibitors, available to help manage symptoms. However, this post isn’t meant to serve as a meal plan or exercise sheet. Instead, we’ve put together a list of hacks that we think can make a difference even if you haven’t fully optimized your health.
- Drink a tablespoon of vinegar ~20 minutes before a meal. This helps avoid spikes in your blood sugar.
- Go for a walk after meals, especially if those meals are heavy on carbs (e.g., pasta, potatoes, bread). This helps your muscles absorb glucose more efficiently.
- Perform at least 10m of vigorous exercise per day. Raising your heart rate (e.g., through a short HIIT session) helps boost your insulin sensitivity, which keeps blood sugar low.some text
- Exercise is most effective at reducing blood sugar spikes when done within an hour before or after a meal
- Eat your carbs last. Start your meal by eating vegetables (which are high in fiber), then eating proteins and fats, and finally moving to carbs. This helps slow the absorption of sugar into your bloodstream, and in turn reduce sugar spikes.
Small steps add up
Although the hacks mentioned above aren’t meant to replace a healthy lifestyle, they can help you make an immediate improvement in your metabolic health and kickstart your dementia prevention efforts. Remember - working on your metabolic health isn’t just about preventing diabetes, it’s about safeguarding your cognitive health.
Actions to consider
- Measure your metabolic markers. Some of these you may get on your annual physical (e.g., HbA1c, HDL-C, LDL-C, glucose, triglycerides, insulin). Others are less common (e.g., Lp(a), ApoB). Most importantly, don’t settle for just ok. These markers are worth optimizing. All the tests mentioned above are part of the 50+ biomarkers tested during your BetterBrain Essentials blood draw.
- Consider using a CGM to get a more accurate view of how your body processes sugar. Using a CGM, you can observe the effects of what you eat and your lifestyle on your blood sugar in real time, which can help inform the daily choices you make. We love the Dexcom G7, which may be challenging to buy over-the-counter but can be bought for cheaper through Signos.
- Learn more about homocysteine on the Peter Attia Drive podcast #252. This episode covers a wide variety of topics related to brain health, and links many different risks and possible interventions to metabolic health.
Get immediate insights with a 3 minute assessment
Start nowShould you get tested for APOE4?
Chance are, you know someone who has tested for their APOE genotype. With the advent of consumer genotyping companies such as 23andme, genetic testing for Alzheimer's risk has become increasingly accessible, with the APOE4 gene variant taking center stage in the discussion. The question that many people are asking is: Should I get tested for APOE4? This article aims to provide a balanced perspective, detailing the pros and cons to help you make an informed decision.
What Is APOE4?
The APOE gene produces a protein essential for fat metabolism and is involved in brain cell repair. There are three main variants of this gene—APOE2, APOE3, and APOE4—with the APOE4 variant being strongly associated with an increased risk of developing Alzheimer's disease. While having this gene variant doesn't guarantee that you'll develop Alzheimer's, it can significantly elevate your risk. 20-25% of people have 1 copy of APOE4, conferring a 2-3X increase in Alzheimer's risk, while 2-3% of people have 2 copies, which implies an 8-10X increase in risk.
Advantages of APOE4 Testing
Empowers You to Make Informed Choices
Perhaps the most compelling reason for getting tested is the ability to make informed decisions about your health. There are specific recommendations for those carrying APOE4 such as significantly increasing DHA consumption given impaired absorption. Additionally, research suggests that APOE4 carriers get even more benefit from a range of interventions than non-carriers. In fact, some experts suggest that by applying the right interventions, you can completely mitigate the impact of having a copy of APOE4.
Opens opportunities for clinical trials and futures therapies
There is a significant research focus on APOE4 and potential pharmacological approaches to mitigating the associated risk. Testing may open up avenues for participating in such trials. Furthermore, as therapies get approved in the future for APOE4 carriers, you'll be well positioned to take advantage.
Offers Information for Family Planning
Your genetic makeup doesn't just affect you; it could also be informative for your family members. Given the heritability of the gene, knowing that you carry the APOE4 variant could give valuable insights into your relatives such as parents who may be at higher risk for developing dementia.
Drawbacks of APOE4 Testing
Carries Emotional and Psychological Weight
Although APOE4 is simply a risk factor and is far from being deterministic, finding out that you're at higher risk for Alzheimer's can be emotionally taxing. While the REVEAL study1 showed that disclosing ApoE4 status did not cause clinically significant anxiety or depression after 6 month follow up, responses are of course very individualized. Before taking the test, consider whether you're emotionally prepared for the results.
Doesn't Guarantee Prevention or Cure
At present, there is no cure for Alzheimer's. Knowing you have the APOE4 gene can offer a sense of urgency to adopt preventive measures, but it doesn't guarantee that you'll be able to ward off the disease.
Raises Ethical and Privacy Concerns
Genetic testing often brings up privacy issues. There's always the risk of data leaks or misuse by third parties, including insurance companies, even though laws exist to prevent genetic discrimination (e.g., GINA for health insurance). Be aware of these concerns when contemplating testing.
The Decision is Yours to Make
Choosing whether to undergo APOE4 testing is a deeply personal decision that should be based on multiple factors, including your emotional readiness, family history, and the current state of your cognitive health. Regardless of your decision, remember that the genetics are just one piece of a very complicated puzzle.

.png)